Prostatakreft er en av de hyppigste kreftformene i Norge, men så langt har ikke de kliniske diagnoseverktøyene kunnet si så mye om hvor i prostata kreften sitter, eller hvor aggressive kreften er i enkeltpasienter. En ny metode utviklet ved MR-senteret kan gi klarere svar.
Ved å kombinere magnetisk resonans avbildning (MRI) med MR spektroskopi (MRS) har PhD kandidat Kirsten Margrete Selnæs utviklet en metode som gjør at man kan si noe om hvor i prostatakjertelen kreften befinner seg, og hvor langt den har kommet. Metoden kan også gi en klarere ide om hvor aggressiv kreften er, noe som er avgjørende for eventuell behandling.
Måler aggressiviteten
– Et av problemene med prostatakreft er å vite hvem som har aggressiv kreft og som trenger behandling, og hvem som kan avvente behandling, sier Selnæs.
Hun brukte to forskjellige MR metoder få å finne svar på spørsmålet om aggressivitet. Først blir vevsprøver fra prostatakjertelen sett på utenfor kroppen (ex vivo). Vevsprøven blir kjørt gjennom et MR spektrometer som gir et spekter eller metabolsk profil. Forskerne ser da etter verdier som skiller seg ut i den kreften som er aggressiv.
I ex vivo testene fant forskerne to mulige biomarkører for prostatakreftaggressivitet: metabolittene citrat og spermin.
Samme test kan så gjøres på pasienter i kroppen (in vivo), men dette gir mindre detaljer. Allikevel fant Selnæs at målingene fra ex vivo testene samsvarer med testene gjort in vivo. Dette kan bety en mer detaljert diagnose før man eventuelt går inn og opererer ut prostata.
– Til nå har vi ikke kunnet skille den aggressive fra den mindre farlige kreften i klinikken, men vi håper nå å være nærmere en metode for å skille disse uten å måtte operere, sier Selnæs.
– Med screening av prostatakreft er det veldig mange som blir oppdaget, men som aldri vil få en sykdom de vil bli plaget av. Så langt har det ikke funnets noen metode for helt sikkert å si hvem som vil dø av kreften, og hvem som kan slippe behandling.
Detaljert kart
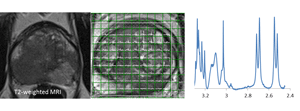
Selnæs har også sammenlignet MRS resultatene med MR bilder for å få en detaljert oversikt over hvor vevsprøvene stammer fra.
Vanligvis når man samler vevsprøver fra prostata tar man en biopsi, og selv om man vet at prøven kommer fra f.eks. høyre eller venstre side av prostata, vet man ikke noe mer.
Ved å kombinere MRI med MRS in vivo i pasienten kan man gi urologen mer presise data for hvor biopsien bør tas – forskjellen er omtrent som å prøve å navigere fra et fotografi sammenlignet med et kart med presise GPS koordinater.
Det man gjør, er å bruke MR bildene til å identifisere områder som ser suspekte ut, og så kjøre MRS tester på disse. Hvis MRS resultatene også viser et typisk «kreft-resultat», kan man være mer sikker på at det faktisk er kreft – man har rett og slett flere bevis.
For å komme fram til dette, brukte Selnæs en ny metode utviklet ved Institutt for Laboratoriemedisin, barne- og kvinnesykdommer (LBK), hvor man kan vite nøyaktig hvor i prostata vevsprøver er samlet fra. Dette gir muligheten for å sammenligne det visuelle bildet fra MR med målingsresultatene man får ved MRS.
Videre forskning
Selv om Selnæs er ferdig med doktorgradsarbeidet, er forskningen på ingen måte omme. Funnene med biomarkørene skal valideres gjennom større pasient studier, og man skal gjennomføre en aktiv overvåkningsstudie med pasienter som etter kliniske vurderinger, kan vente med behandling.
– Vi vil ta MR når de blir inkludert i studien, og etter ett år når de har rutinekontroll. Og så vil vi se om det er noe i MR bildene eller MR spektrene som kan si noe om hvem som fortsatt bør overvåkes, forklarer Selnæs.
Disputas
Kirsten Margrete Selnæs disputerer 25. september 2012, kl. 12.15 i Auditoriet, Medisinsk teknisk forskningssenter (MTFS).
I forbindelse med disputasen avholdes et seminar om prostatakreft og MR dagen før, 24. september.
Relaterte publikasjoner
- Discrimination of patients with microsatellite instability colon cancer using 1H HR MAS MR spectroscopy and chemometric analysis.
- Quality control of prostate (1) H MRSI data.
|
Magnetisk resonans avbildning (MRI) er en metode for å ta snitt-bilder av deler av kroppen ved hjelp av radiobølger og magnetfelt uten kjente biologiske skadevirkninger.
Magnet resonans spektroskopi (MRS) er en metode for å se på metabolismen (stoffskiftet) i celler og gir informasjon om cellens biokjemiske reaksjoner. Metabolitter er molekyler som tar del i, eller lages av, stoffskiftet i cellene. Prostatakreft er en ondartet svulst i prostatakjertelen og er den vanligste kreftformen blant menn i Norge. |